By Sophie Davis-Cooper on November 16, 2022
In our recent survey of over 2,000 adults across the UK, we found a disconnect between the public’s understanding of the concept of virtual wards and the phrase itself. 53% would prefer to have their health monitored from home than in hospital, but this enthusiasm almost halves when the term ‘virtual ward’ is used.
Patient engagement and adoption is crucial to the long-term success of virtual wards. But how can they embrace something they don’t understand? That was the topic of conversation for our panel of frontline clinicians on our recent webinar.
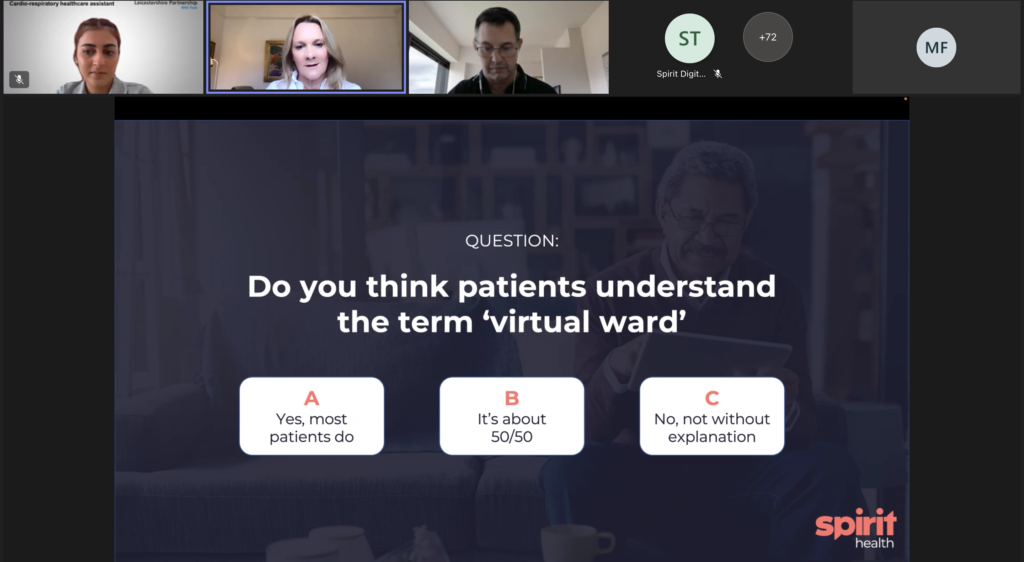
The session started with a simple question to the audience: Do you think patients understand the term virtual wards? Echoing the public survey findings, 91% answered ‘no, not without explanation’. So how can we better explain what a virtual ward is?
Onboarding is important
Johnny Wells, Lead Matron, Emergency Department at Norfolk and Norwich University Hospitals, said his experience of onboarding patients onto virtual wards reflected the results. “I spend a lot of my time onboarding patients and giving them clear descriptions and myth busting, because when you actually say, ‘Have you heard of a virtual ward?’ Of course not, it’s new to them.”
Aleesha Karia, Healthcare Assistant and part of the virtual ward onboarding team at Leicestershire Partnership NHS Trust, also witnessed initial resistance from patients.
“… they immediately say ‘Well, I’m not that confident with technology’, and they assume you’d have to be a technical whiz to be able to get onto the platform. But I think once you explain it, how easy it is, that it’s just a website that’s used for communication purposes, they’re very much onboard for it.”
– Aleesha
The elevator pitch
When it comes to explaining what a virtual ward is, Johnny shared his ‘elevator pitch’ for patients.
“I would say, ‘I’ve got a new way of actually getting you home. You’re still going to have the level of care that you receive as an inpatient, you will still be safe and monitored. It’s more bespoke and tailored to you. You will be back in front of your own telly, with your family and pets’. Everything’s a win.”
– Johnny
Jane Van Aken, Director of Service Development at Spirit Health and registered nurse, added that it’s “important for patients to know there’s a doctor’s name above each virtual bed.” This reassures patients that they are still under the care of the hospital team even after they’ve left the building.
Aleesha said she would usually refer to virtual wards as a ‘website’ since most people recognise that concept. “My first opening line would be, ‘it’s a website on the internet that nurses will communicate to you on’. And there’s a nursing team behind the screen; you’re not alone. I’ve had patients say they felt they’ve had more access to their clinical team because they have this connection.”
“We use the word Google, we use the word Uber, along with other tech products as common verbs in our society. So, there’s no reason why ‘virtual ward’, when explained properly, couldn’t become embedded in healthcare.”
– Jane
Success stories
Johnny emphasised the importance of using patients’ success stories to help ‘sell’ the benefits of virtual wards.
“I had a patient who was reluctant because they didn’t understand the concept. I had another patient using the virtual ward, who was really impressed with the service and he thought the one-to-one communication was very personal. So, I called him.
By the patient’s bedside, I video-called the virtual ward patient and held up the tablet so they could talk. And he sold it for me, he just said, ‘Trust them, it will get you home. You’re going to eat better; you’ll be in your own bed. Why would you want to stay in the hospital when you can be at home with your family?’
That’s where patient testimonials and feedback is really powerful for us all.”
– Johnny
Family support
Involving patient’s families and carers in the onboarding process can also boost confidence. Aleesha shared how involving loved ones helped overcome digital literacy and language barriers for certain patients.
“I think one of the main challenges is the digital literacy in some patients and they need additional support. So, we like to get families involved. When there’s a language barrier or just difficulty in using the technology, there’s usually someone in the family who would love to facilitate this care. This can relieve their own anxiety knowing there’s a nurse taking care of their family member or loved one.”
– Aleesha
Engaging clinicians
Jane reminded us that clinical buy-in is just as important as patient buy-in. If the healthcare team haven’t fully embraced virtual wards, how can their patients?
When talking to fellow nurses, she refers to it as a ‘tool in our toolbox’.
“We know it’s not replacing us, it’s just helping us do our job better, be more efficient, make better clinical decisions, have more time for those patients who really need to see us.”
– Jane
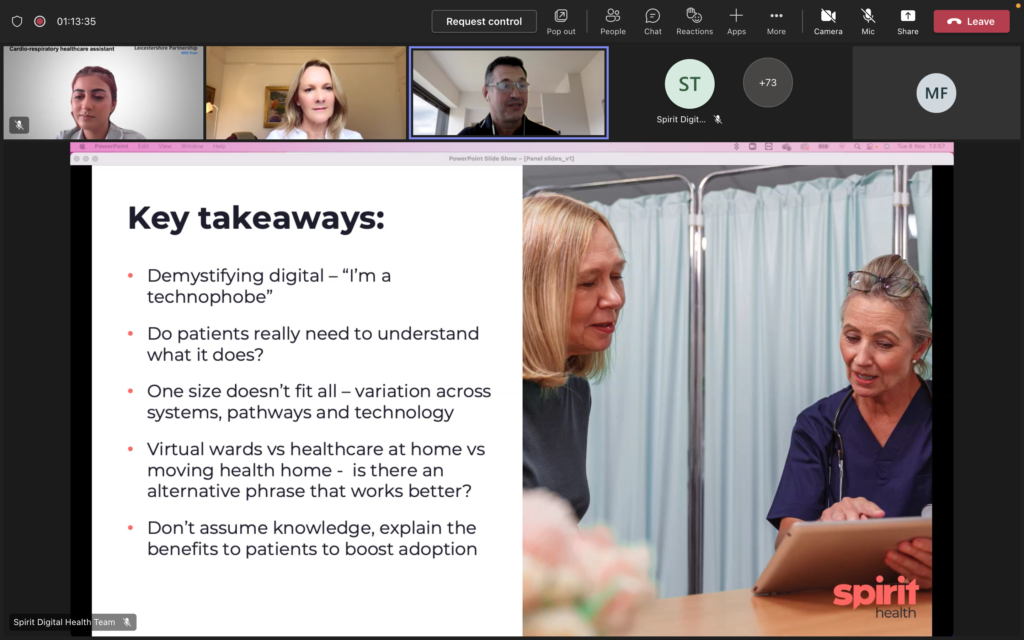
Key takeaways from the panel
- Don’t assume knowledge
As the survey found, most people are unfamiliar with the term ‘virtual wards’ so clinicians need to ensure the service is clearly explained in language that patients understand. Leading the conversation with the benefit rather than the concept can be more effective. For example, “I’ve got a plan to get you home”. - Use patient stories
Nothing is more powerful than hearing patient stories. Listening to other people who have gone through a similar experience can help patients overcome their initial concerns. If they can do it, why can’t I? - Engage family and carers
Involving the family and carers in the onboarding process can boost confidence and ease anxiety, both for the patient and for their loved ones. - Onboard clinical teams
The healthcare professionals onboarding patients need to be champions of virtual wards. Patients will never be willing to try something new unless it’s backed by the people they trust.
Missed the session? You can watch the full recording here: